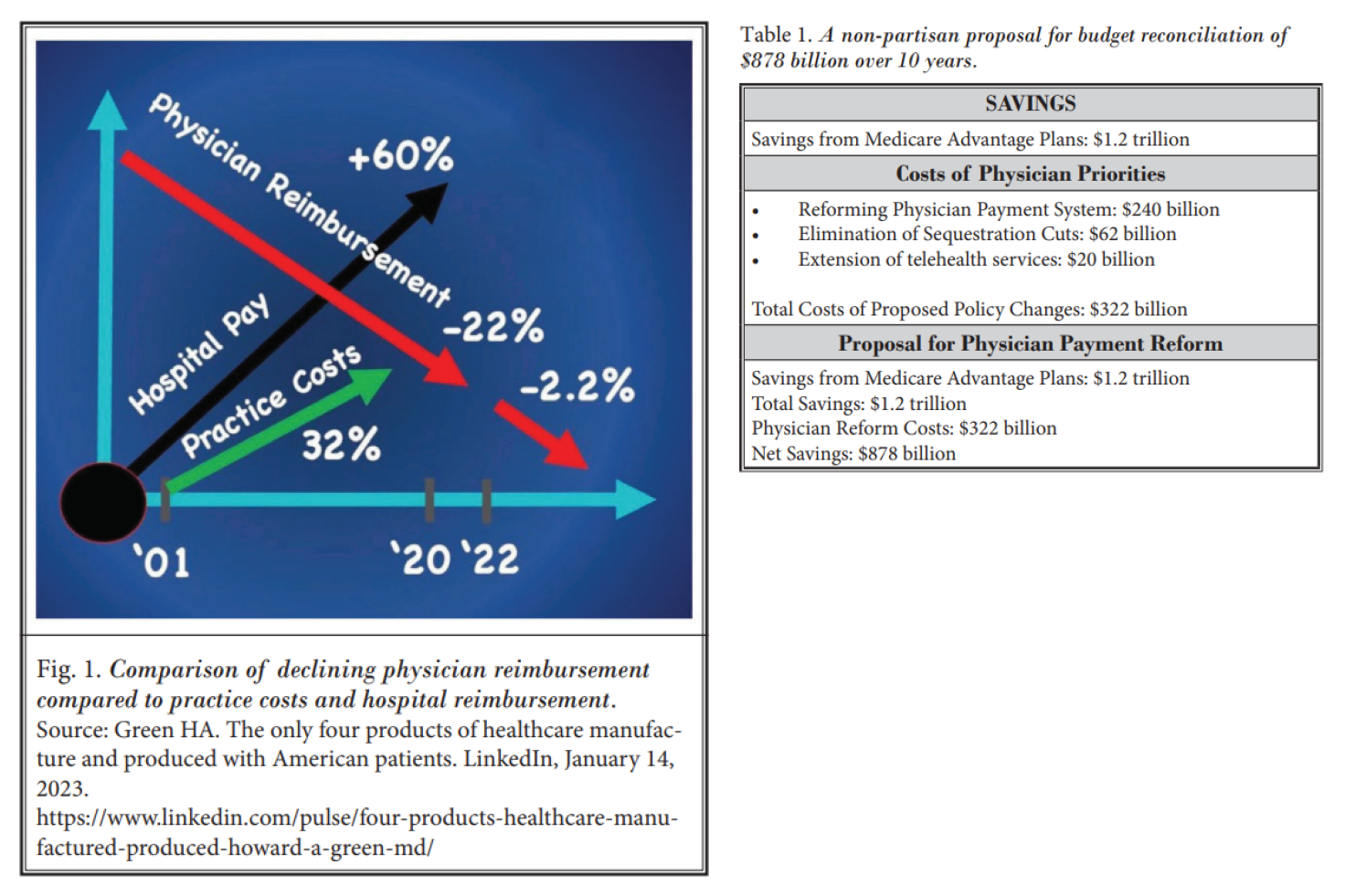
Physician payments have declined significantly due to budget neutrality rules and reimbursement cuts. Since 2001, Medicare payments to physicians have dropped by 33% when adjusted for inflation. These reductions have been compounded by 2% annual sequestration cuts introduced after the Affordable Care Act (ACA), which continues through 2032. Despite their long-term impact, sequestration cuts receive little public attention.
Congress has historically delayed or softened these cuts. However, in 2025, a bill that would have adjusted payment rates was removed from the continuing resolution, resulting in continued reductions. Meanwhile, insurance premiums have risen nearly 400%, highlighting the disparity
between healthcare costs and physician compensation.
Ironically, while physicians face significant payment cuts, the Centers for Medicare & Medicaid Services (CMS) proposed on January 10, 2025, a 4.3% payment increase for Medicare Advantage plans—totaling $21 billion in 2026 and an estimated $210 billion over the following decade starting in calendar year 2026. This proposal comes amid ongoing concerns about Medicare Advantage overpayments, estimated at nearly $100 billion annually, and additional funding through annual
premiums of $198 from all Medicare beneficiaries, amounting to roughly $13 billion per year.
In response, the American Society of Interventional Pain Physicians (ASIPP) submitted a nonpartisan reform proposal advocating for telehealth protections and elimination of sequester cuts—measures that have received strong bipartisan support in Congress.
Both the House of Representatives and the Senate voted to pass a reconciliation bill—nicknamed the “Big Beautiful Bill”, which has been signed into law by the President recently.
It proposes an $8.9 billion investment in the Medicare Physician Fee Schedule, with a 2.25% update in 2026.
The proposal does not address the budget neutrality provision, growing practice costs, inflationary pressures, or ongoing sequestration and pay-as-you-go (PAYGO) cuts. It also fails to resolve issues with the Medicare Access and CHIP Reauthorization Act (MACRA), particularly within the Merit-Based Incentive Payment System (MIPS).
On November 1, 2024, CMS finalized a 2.8% cut to physician payments—an estimated $20 billion—while also eliminating telehealth services. These cuts continue to threaten physician sustainability and patient access to care.
📄 Read the full Pain Physician Journal article here: https://www.painphysicianjournal.com/current/pdf?article=ODAyNA%3D%3D
